Vagal Nerve Stimulation
Vagal Nerve Stimulation
Vagal Nerve Stimulation
A vagal nerve stimulator (VNS) is an electronic device that, once turned on, delivers gentle electrical pulses to the brain. A brain surgeon implants the VNS device during a less-invasive procedure.
For some people, a VNS can improve symptoms of depression, epilepsy, or upper arm weakness from a stroke. It may be an option when other treatments are no longer working.
At Carilion Clinic, we're proud to have been the first in Virginia to offer VNS implants to treat epilepsy. We currently use this technology for several brain-related conditions. We offer this specialized support to those who need it most.
A vagal nerve stimulator (VNS) is an electronic device that, once turned on, delivers gentle electrical pulses to the brain. A brain surgeon implants the VNS device during a less-invasive procedure.
For some people, a VNS can improve symptoms of depression, epilepsy, or upper arm weakness from a stroke. It may be an option when other treatments are no longer working.
At Carilion Clinic, we're proud to have been the first in Virginia to offer VNS implants to treat epilepsy. We currently use this technology for several brain-related conditions. We offer this specialized support to those who need it most.
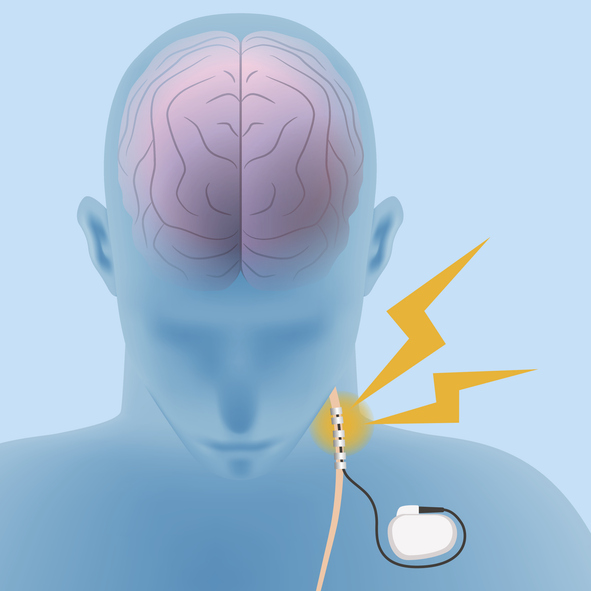
The vagus nerve is one of 12 cranial nerve pairs that start in the brain and connect to different body parts. The vagus nerve plays a role in sensory and motor functions and is vital to the autonomic nervous system.
It starts in the brain, travels down the neck, and connects to several organs. These include the heart, stomach, and lungs. This nerve controls body functions like heartbeat, breathing, and digestion.
The VNS is a small, pacemaker-like device. A surgeon inserts it under the skin of the upper chest and connects it to the vagus nerve via a thin wire in the neck. The device controls seizures by sending mild electrical pulses through the vagus nerve to the brain.
These pulses can influence brain function without requiring any direct brain surgery. By altering brain pathways, these pulses help manage:
- Medication-resistant epilepsy
- Treatment-resistant depression
- Stroke-related movement issues
Most patients can’t feel the stimulation, but it can help their symptoms and quality of life.
What Is Vagal Nerve Stimulation?
The vagus nerve is one of 12 cranial nerve pairs that start in the brain and connect to different body parts. The vagus nerve plays a role in sensory and motor functions and is vital to the autonomic nervous system.
It starts in the brain, travels down the neck, and connects to several organs. These include the heart, stomach, and lungs. This nerve controls body functions like heartbeat, breathing, and digestion.
The VNS is a small, pacemaker-like device. A surgeon inserts it under the skin of the upper chest and connects it to the vagus nerve via a thin wire in the neck. The device controls seizures by sending mild electrical pulses through the vagus nerve to the brain.
These pulses can influence brain function without requiring any direct brain surgery. By altering brain pathways, these pulses help manage:
- Medication-resistant epilepsy
- Treatment-resistant depression
- Stroke-related movement issues
Most patients can’t feel the stimulation, but it can help their symptoms and quality of life.
A VNS is an option if your symptoms haven't improved with other treatments. You need to be over 18 and have tried 4 or more medicines without success.
Epilepsy
The FDA approved a vagal nerve stimulation to treat epilepsy in 1997. A VNS implant may be an option if you haven't found adequate relief from other medicines. It may help reduce your seizure frequency and improve recovery after seizures.
Vagal nerve stimulation isn’t always fully effective. It doesn’t replace medicine. However, it can reduce seizure frequency, severity, and recovery time after a seizure. It can take up to 2 years to affect seizures.
Many report better control, fewer ER visits and improved well-being after getting a VNS implanted. It can improve mood, memory, and cognitive skills and enhance their quality of life.
Treatment-resistant depression
If you have chronic depression, and medicines and therapy aren't helping, vagal nerve stimulation may offer relief. The stimulation may trigger the brain to make more of the brain chemicals that combat depression.
The FDA approved vagal nerve stimulation for treatment-resistant depression in 2005. Over time, a VNS implant can lead to a reduction in symptoms. While it may take several months to see effects, up to 30% of patients report significant symptom relief after a year of treatment. Over longer time frames, symptom relief can continue to improve.
More than half of people who get a VNS for depression report an enhanced quality of life. They also see long-term symptom management.
Stroke recovery
If you’ve had a stroke and, after years of recovery, still have limited arm and hand movement, a VNS might help. It, combined with occupational therapy, may help restore movement.
Vagal nerve stimulation for stroke recovery can strengthen the links in the brain and improve motor function. Patients will often see better mobility and increased ability to perform daily tasks. This gives them an improved sense of independence and well-being.
Is Vagal Nerve Stimulation Right for Me?
A VNS is an option if your symptoms haven't improved with other treatments. You need to be over 18 and have tried 4 or more medicines without success.
Epilepsy
The FDA approved a vagal nerve stimulation to treat epilepsy in 1997. A VNS implant may be an option if you haven't found adequate relief from other medicines. It may help reduce your seizure frequency and improve recovery after seizures.
Vagal nerve stimulation isn’t always fully effective. It doesn’t replace medicine. However, it can reduce seizure frequency, severity, and recovery time after a seizure. It can take up to 2 years to affect seizures.
Many report better control, fewer ER visits and improved well-being after getting a VNS implanted. It can improve mood, memory, and cognitive skills and enhance their quality of life.
Treatment-resistant depression
If you have chronic depression, and medicines and therapy aren't helping, vagal nerve stimulation may offer relief. The stimulation may trigger the brain to make more of the brain chemicals that combat depression.
The FDA approved vagal nerve stimulation for treatment-resistant depression in 2005. Over time, a VNS implant can lead to a reduction in symptoms. While it may take several months to see effects, up to 30% of patients report significant symptom relief after a year of treatment. Over longer time frames, symptom relief can continue to improve.
More than half of people who get a VNS for depression report an enhanced quality of life. They also see long-term symptom management.
Stroke recovery
If you’ve had a stroke and, after years of recovery, still have limited arm and hand movement, a VNS might help. It, combined with occupational therapy, may help restore movement.
Vagal nerve stimulation for stroke recovery can strengthen the links in the brain and improve motor function. Patients will often see better mobility and increased ability to perform daily tasks. This gives them an improved sense of independence and well-being.
At Carilion, we tailor our vagal nerve stimulation approach to you, your condition, and your brain. Our dedicated nurse navigator coordinates every step of your care. They’re by your side from initial visits to answering questions after surgery.
Before
You’ll meet with our neurologists and brain surgeons to find out if you’re a candidate for vagal nerve stimulation. They'll review your medical history and do tests to determine whether this device is a good option for you.
Pre-surgical evaluations may include imaging studies of your brain. You’ll also visit with neurology and psychology experts. A VNS device is precision medicine; we tailor the implantation procedure based on your unique condition.
During implantation
A brain surgeon does the VNS implant procedure under general anesthesia. It takes less than 90 minutes.
This surgery involves 2 small incisions. An incision in your upper-left chest is where the surgeon implants the pulse generator. The incision in your left lower neck is for the wire connection to the vagus nerve.
After the procedure
After the VNS implant surgery, most patients go home within 24 hours. You’ll have follow-up visits to activate and adjust the VNS device settings over the next several months.
Your neurologist will activate the VNS device 2 to 4 weeks after the surgeon implants it. The treating neurologist programs the stimulator in their office. They test out different strengths and durations of the electrical impulses. Patients with epilepsy or depression may notice improvements over months.
People using a VNS device for stroke recovery will get occupational therapy for 6 weeks. During therapy sessions, the device will deliver a gentle pulse to the vagus nerve. At the same time, the patient performs a functional task, such as cutting food or buttoning a shirt. Pairing the action and stimulation creates and strengthens connections in the brain.
What Should I Expect?
At Carilion, we tailor our vagal nerve stimulation approach to you, your condition, and your brain. Our dedicated nurse navigator coordinates every step of your care. They’re by your side from initial visits to answering questions after surgery.
Before
You’ll meet with our neurologists and brain surgeons to find out if you’re a candidate for vagal nerve stimulation. They'll review your medical history and do tests to determine whether this device is a good option for you.
Pre-surgical evaluations may include imaging studies of your brain. You’ll also visit with neurology and psychology experts. A VNS device is precision medicine; we tailor the implantation procedure based on your unique condition.
During implantation
A brain surgeon does the VNS implant procedure under general anesthesia. It takes less than 90 minutes.
This surgery involves 2 small incisions. An incision in your upper-left chest is where the surgeon implants the pulse generator. The incision in your left lower neck is for the wire connection to the vagus nerve.
After the procedure
After the VNS implant surgery, most patients go home within 24 hours. You’ll have follow-up visits to activate and adjust the VNS device settings over the next several months.
Your neurologist will activate the VNS device 2 to 4 weeks after the surgeon implants it. The treating neurologist programs the stimulator in their office. They test out different strengths and durations of the electrical impulses. Patients with epilepsy or depression may notice improvements over months.
People using a VNS device for stroke recovery will get occupational therapy for 6 weeks. During therapy sessions, the device will deliver a gentle pulse to the vagus nerve. At the same time, the patient performs a functional task, such as cutting food or buttoning a shirt. Pairing the action and stimulation creates and strengthens connections in the brain.
VNS implants are generally safe. As with any surgical procedure, there are potential risks and side effects. These are mild and related to the stimulation, improving over time.
Common side effects include:
- Hoarseness
- Throat irritation
- Shortness of breath
- A dry cough
Other less-frequent side effects can include:
- Headaches
- Mild pain
- Insomnia
- Tingling sensations
Changing the device settings can help reduce side effects.
Risks of Vagal Nerve Stimulation
VNS implants are generally safe. As with any surgical procedure, there are potential risks and side effects. These are mild and related to the stimulation, improving over time.
Common side effects include:
- Hoarseness
- Throat irritation
- Shortness of breath
- A dry cough
Other less-frequent side effects can include:
- Headaches
- Mild pain
- Insomnia
- Tingling sensations
Changing the device settings can help reduce side effects.
Our brain surgeons use VNS implants to treat the most complex, medically refractory epilepsy and depression. We use the latest generation of procedures and implants.
Pioneers in Virginia
We were the first clinic in Virginia to offer VNS implants for treatment-resistant depression.

Dedicated nurse navigators
Our nurse navigators guide you through each step of the process. They’re by your side from pre-surgery testing to post-implant follow-up.

Commitment to care
Carilion offers ongoing support and expertise. We help patients achieve the best possible outcomes for our VNS implant patients.
Why Choose Carilion Clinic?
Our brain surgeons use VNS implants to treat the most complex, medically refractory epilepsy and depression. We use the latest generation of procedures and implants.
Health and Wellness
Improving Stroke Outcomes With Technology

Stroke in Young People: What You Need To Know
A Day in the Life: Neurosurgery Residents
Get Care at Carilion Clinic
Your path to better health starts here. Explore comprehensive care options and find the support you need for every step of your wellness journey.
Get Care at Carilion Clinic
Your path to better health starts here. Explore comprehensive care options and find the support you need for every step of your wellness journey.
Get Care at Carilion Clinic
Your path to better health starts here. Explore comprehensive care options and find the support you need for every step of your wellness journey.
Get Care at Carilion Clinic
Your path to better health starts here. Explore comprehensive care options and find the support you need for every step of your wellness journey.

